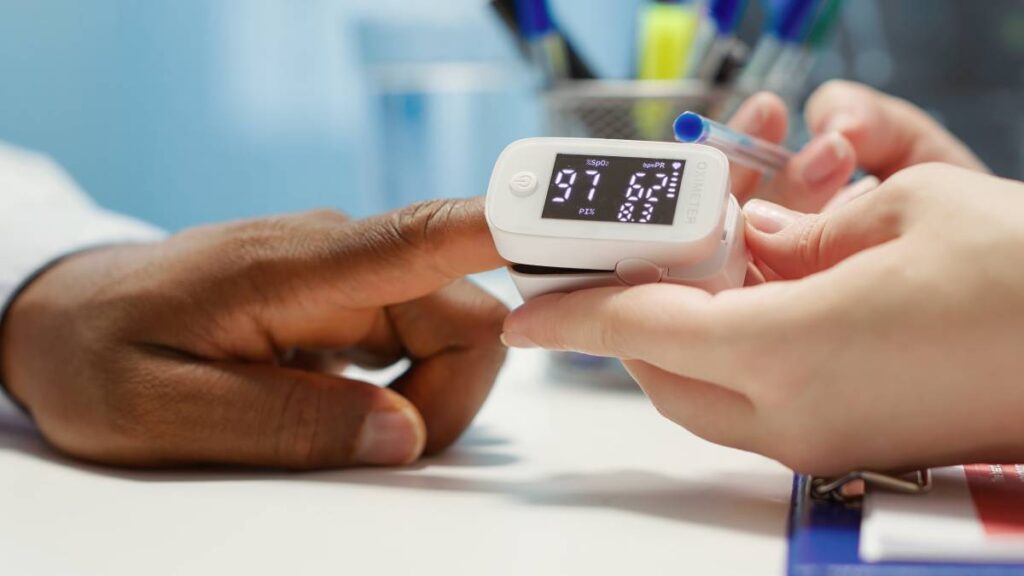
Pulse oximeters are devices that estimate the percentage of oxygen in the blood. Widely used in clinical settings, these tools have experienced growth in at-home usage since the COVID-19 pandemic. However, many people are unaware that their accuracy can vary based on skin tone.
To assess the blood’s oxygen content, a pulse oximeter shines light through the skin. It uses two wavelengths of light—red and infrared—and measures how much is absorbed as blood pulses through the tissue. In principle, this method is simple and noninvasive, but in practice, it can be affected by the way light interacts with different pigments, including melanin. Depending on how the pulse oximeter was designed and tested, this may result in people with darker skin tones receiving readings that are less accurate than readings for people with lighter skin.
Research over the past several years has shown a consistent pattern: pulse oximeters tend to overestimate oxygen levels in individuals with darker skin tone. In particular, the device may display a normal or near-normal oxygen saturation reading when the true level is lower. This phenomenon became more widely recognized during the pandemic, when clinicians noticed that some patients of color appeared stable based on their pulse oximeter numbers yet were actually experiencing more severe oxygen deprivation than the device indicated.
This discrepancy is not a minor issue. For people with respiratory illnesses, timely recognition of low oxygen levels can influence when they seek care, how they are treated in emergency settings, and the urgency of interventions like supplemental oxygen or hospitalization.
Skin tone influences pulse oximeter readings due to the way in which melanin absorbs light. Because darker skin contains more melanin, more light in the wavelengths used by pulse oximeters is absorbed, potentially producing a misleadingly elevated reading. Since many devices rely on preset algorithms that were originally calibrated using mostly light-skinned individuals, the results may not account for the full range of optical differences. While modern pulse oximeters are more sophisticated than earlier generations, many still carry the same bias because their foundational design has not changed. Manufacturers and regulators are now paying more attention to these concerns, but improvements take time.
For the average person using a pulse oximeter at home, this issue does not mean the device is useless. It does, however, mean that readings should be interpreted with some caution, particularly if the user has a darker skin tone.
A single measurement should not be the only factor guiding decisions about health. Symptoms such as shortness of breath, chest discomfort, unusual fatigue, bluish lips, or worsening cough are often more reliable indicators that something is wrong. If the pulse oximeter shows borderline or slightly normal values but symptoms appear severe, it is important to trust those symptoms and seek medical advice promptly. In clinical settings, healthcare providers can obtain more accurate results with other tests, especially in patients who are at risk of respiratory complications or for whom oxygenation status is vital to monitor.
The growing recognition of skin-tone bias in medical devices has sparked broader conversations about equity in healthcare design. Pulse oximeters were never intentionally engineered to be less accurate for certain groups, yet the oversight reflects a larger pattern in which technologies are developed and tested using limited populations. Improving these devices will require more inclusive testing, updated algorithms, and regulations that demand accuracy across diverse skin tones. Some newer devices and research prototypes are already being designed with these factors in mind, signaling progress toward more reliable readings for everyone.
Understanding the limitations of pulse oximeters helps users make better decisions. These devices remain helpful tools for monitoring trends in oxygen levels, but they are not perfect, and their imperfections affect some people more than others. By recognizing the role skin tone can play in readings, individuals and healthcare providers can approach their use with greater awareness and ensure that concerns about oxygen levels are evaluated as safely and accurately as possible.